Low access and coverage for the treatment of acute malnutrition is as persistent and perplexing as it is unacceptable. The leading barriers to combatting malnutrition—distance to services and high opportunity costs—require a new approach.
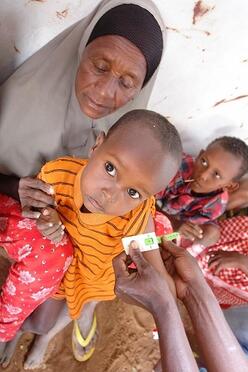
The child health community, through the integrated community case management (iCCM) of childhood illnesses strategy, has improved access to treatment for pneumonia, diarrhea, and malaria by enabling treatment outside of traditional health facilities through a large network of community health workers (CHWs). Since 2014, the International Rescue Committee (IRC) has been exploring a treatment algorithm and tools to empower low-literate providers and bring severe acute malnutrition treatment, without complications, directly to malnourished children in their villages.
This journey, which began in 2015, has included numerous patient registers, dozens of modified mid-upper arm circumference (MUAC) tapes, and partnerships with CHWs, designers, and experts in nutrition and iCCM. A year later, we have the results of the third and most recent field test, which took place in South Sudan. Based on our findings, the IRC believes providing treatment for acute malnutrition outside the facility is possible, understanding that there is still work to be done.
In addition to South Sudan, the IRC began developing and field-testing low-literacy tool prototypes in Mali, Chad, and India in 2015. In the recently wrapped field test in South Sudan, the IRC nutrition and iCCM teams—along with a human-centered design firm called Quicksand—worked with 30 low-literate female iCCM CHWs of varying ages and experience in Aweil South County in Northern Barh El Gazal State.
The process focused on capturing the end-user perspective. Each group of CHWs trained on the prototypes and participated in all three rounds. During each round, the CHWs practiced using the tools while being observed by the IRC and Quicksand team. At the end of each round, CHW feedback was solicited on each of the tools. For two rounds, CHWs worked with children enrolled in the outpatient therapeutic program.
A number of key results emerged in the process of developing and testing the tools:
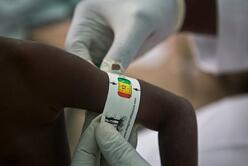
- Low-literate CHWs can correctly take MUAC to admit, follow up, and discharge children. To reduce the amount of decision making for a CHW, a new dark red zone was added to the MUAC tape for referral of critical cases, modeled after the dark red shade that signals a danger sign for iCCM in South Sudan. Across the board, CHWs preferred the dark red shade, finding it easy to remember as a ‘danger sign’ requiring referral to the nutrition stabilization center, therein simplifying the decision-making burden on the CHW for these critical cases. Since CHWs are already trained to take MUAC for referral they had no problem then doing so correctly. A key issue of monitoring progression and regression still remains and new prototypes are being explored by the IRC–Quicksand team to solve this issue.
- Low-literate CHWs can correctly determine the daily and weekly dosage of ready-to use therapeutic food (RUTF). To ensure CHWs could easily determine the correct dosage of RUTF for patients each week, the IRC–Quicksand team simplified the standard RUTF look-up table and developed a corresponding dot scale to represent the daily dosage for each weight zone, as derived from the simplified RUTF look-up table. To calculate the weekly dosage, a bag with seven pockets was developed whereby CHWs would fill each pocket with the daily dosage.
- Low-literate CHWs can monitor treatment by using a low-literacy register. The patient register that IRC and Quicksand developed is able to 1) track a patients MUAC reading each week 2) the course of treatment provided 3) include a calculation of performance indicators, and 4) provide a method of providing a connection between the patient and the record for that patient, since CHWs may not be able to write the name of the child. This register required, for example, the development of icons for performance indicators, like sex and age, recovery, death, defaulting, non-response, and transfer that were both understandable and culturally appropriate. The register must also track whether a patient is progressing, stationary or regressing, which is still an issue under exploration.
- Low-literate CHWs can use a child–record identification system to link the child to his or her record. The result was a unique identifier on each patient register sheet and the same identifier on the patient’s card. When the patient card was torn off and given to the child’s caretaker, the caretaker would return with the card and the CHW would match it to the correct record in the register.
Going forward, the IRC is planning to conduct another round of field testing to make a final decision on the toolkit. The IRC also intends to conduct research on the effectiveness of the simplified toolkit and begin collaborating with other organizations interested in piloting the tools.
This project was funded with UK aid from the UK government